- Emergency Line:(+91) 9555943636
- Mon - Fri: 9:00 am - 5:00 pm (24x7 Emergency)
- 8 Marla, Model Town, Sonipat, Haryana 131001
Cardiac Care: Consult the Leading
Cardiologist in Sonipat | Primax Hospital
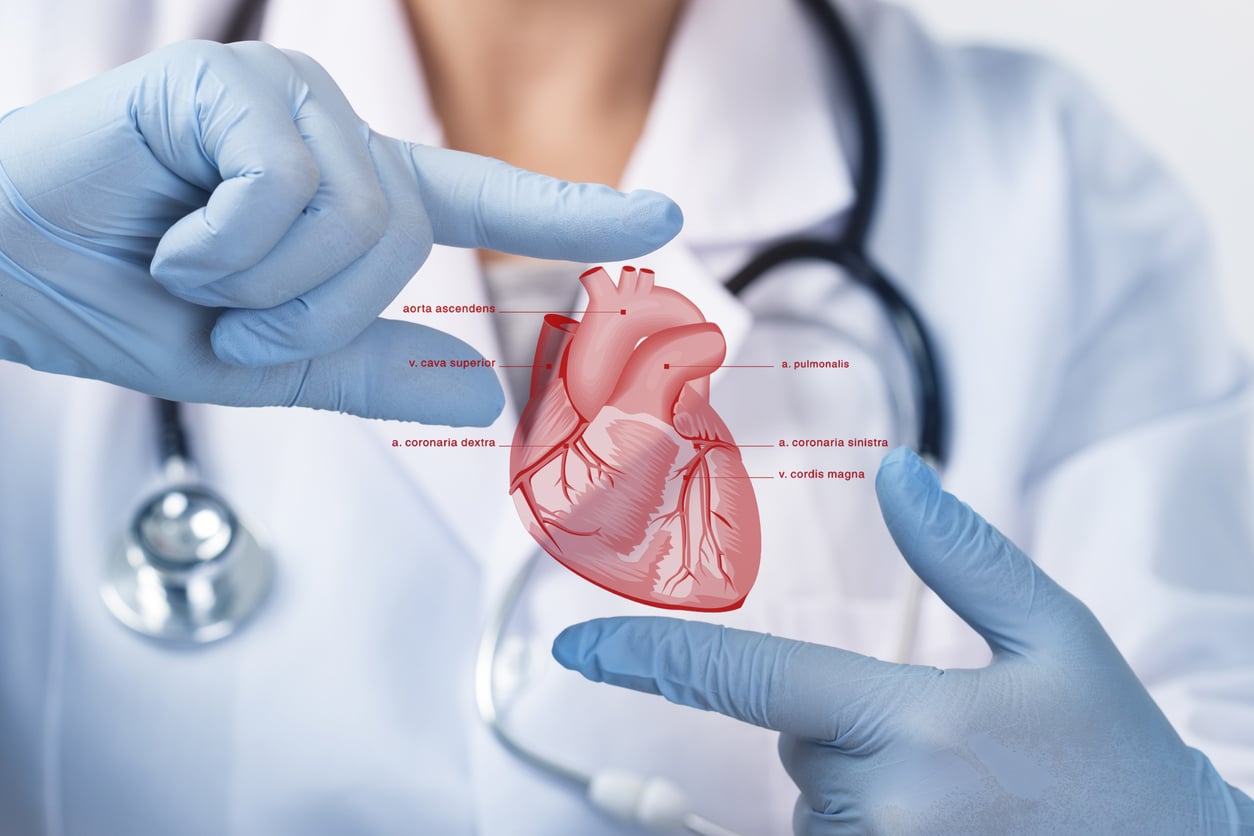
✅ Comprehensive Cardiac Expertise
✅ State-of-the-Art Cardiac Infrastructure and Technology
✅ Rapid Response & Minimally Invasive Procedures
✅ Patient-Centric Cardiac Care
Your heart valves regulate blood flow. When they become narrow (stenosis) or leaky (regurgitation), the heart works harder. Our expert cardiologist in Sonipat provides advanced diagnosis and treatment for all valve disorders.
Valve disease can occur due to aging, infections, congenital issues, or rheumatic fever. If untreated, it may lead to heart failure. Early detection is essential.
What is Angina? Angina occurs when your heart muscle doesn’t receive enough oxygen-rich blood, usually due to narrowed or blocked coronary arteries. While angina itself isn’t a heart attack, it significantly increases your risk of having one. Think of angina as your heart’s way of crying out for help—it’s crucial not to ignore these warning signals.
Classic Angina Symptoms:
Note: Women’s Angina Symptoms May Differ
Women often experience unusual fatigue, sleep disturbances, nausea, and upper back or jaw pain without typical chest pain.
A. Thorough Diagnostic Evaluation:
B. Medical Management for Stable Angina:
C. Interventional Treatment Options:
📞 Don’t Ignore Chest Pain
If you experience chest pressure or discomfort, get evaluated immediately by our cardiac care specialists at Primax Gastro Institute & Super Speciality Hospital.
Call 9666460009 for an urgent angina evaluation.
Peripheral Artery Disease affects arteries outside the heart, most commonly in the legs.
P A D occurs when arteries supplying blood to your limbs (usually legs) become narrowed or blocked due to plaque buildup. This reduces blood flow, causing symptoms during walking and potentially leading to non-healing wounds, gangrene, or amputation if severe and untreated. PAD is also a marker of widespread atherosclerosis affecting coronary and carotid arteries.
A. Intermittent Claudication:
B. Advanced PAD (Critical Limb Ischemia):
A. Diagnostic Evaluation:
B. Medical Management:
C. Supervised Exercise Therapy:
D. Minimally Invasive Interventions:
📞 Don’t Ignore Leg Pain When Walking
Contact Primax Gastro Institute & Super Speciality Hospital at 9666460009 for a complete PAD evaluation.
Our Specialized Cardiac Tests
An Electrocardiogram (ECG or EKG) is a crucial test to evaluate your heart’s electrical activity. It is quick, painless, and provides vital information about heart rhythm, heart rate, and signs of heart disease. Our cardiac care department performs hundreds of ECGs daily with expert interpretation.
Process: An ECG records electrical signals generated by your heart. Small electrodes are attached to your chest, arms, and legs. These detect impulses and create a graph showing your heart’s rhythm pattern. This simple test can detect heart attacks, arrhythmias, chamber enlargement, and other abnormalities within minutes.
A. Preparation:
B. During the Test:
C. Results:
Normal ECG Example: “Normal sinus rhythm, 70 bpm, normal axis, no ST-T changes.”
Abnormal ECG Examples:
PTCA (Percutaneous Transluminal Coronary Angioplasty) with stenting is a minimally invasive procedure that opens blocked coronary arteries and restores blood flow to your heart. Our expert cardiologist in Sonipat has performed thousands of successful angioplasties, saving lives and preventing heart attacks.
Angioplasty is a catheter-based procedure where a small balloon is inflated inside a blocked coronary artery to widen it. A stent (tiny mesh tube) is then placed to keep the artery open permanently. This procedure is performed through a small puncture in your wrist or groin artery where no chest opening required.
| Stage | What Happens | Duration |
|---|---|---|
| Pre-Procedure | Fasting, IV line, groin/wrist preparation, consent | 30-60 minutes |
| During Procedure | Local anesthesia, catheter insertion, blockage opened, stent placed | 30-90 minutes |
| Immediate Post-Procedure | Pressure applied to puncture site, monitoring in recovery | 4-6 hours |
| Hospital Stay | Observation, medications started, activity restrictions | 24-48 hours |
| Recovery at Home | Gradual return to activities, follow-up appointments | 1-2 weeks |
If you’ve been diagnosed with coronary artery blockages or are experiencing angina, consult our interventional cardiologists at Primax Gastro Institute & Super Speciality Hospital. Call [9666460009] for appointment or emergency angioplasty services available.
The Treadmill Test (TMT), also called Exercise Stress Test, evaluates how your heart performs under physical stress. It’s one of the most important tests to detect coronary artery disease, assess exercise capacity, and determine if chest pain is cardiac-related.
During TMT, you walk on a treadmill while your heart rate, blood pressure, breathing, and ECG are continuously monitored. The treadmill speed and incline gradually increase, making your heart work progressively harder. This stress reveals problems with blood flow that might not be apparent when you’re resting.
Your Cardiologist Orders TMT To:
| Test Result | ECG Findings | Symptoms |
|---|---|---|
| Negative | No ST changes, good exercise capacity | No chest pain |
| Positive | ST depression ≥1mm, early onset | Chest pain during test |
| Inconclusive | Submaximal heart rate achieved | Non-specific symptoms |
| High-Risk Positive | ST depression ≥2mm, low workload, hypotension | Severe symptoms |
Pacemakers and Implantable Cardioverter-Defibrillators (ICDs) are life-saving devices for patients with heart rhythm disorders. A pacemaker prevents dangerously slow heart rates, while an ICD protects against sudden cardiac death from fatal arrhythmias.
A pacemaker is a small device implanted under the skin (usually below the collarbone) that sends electrical signals to keep your heart beating at a proper rate. It monitors your heart rhythm 24/7 and paces only when needed, allowing natural heart rhythm when present.
An ICD is similar to a pacemaker but also monitors for dangerous rapid rhythms (ventricular tachycardia/fibrillation). If detected, it delivers a shock to restore normal rhythm, preventing sudden cardiac death. Many ICDs also have pacemaker functions.
| Device Type | Function | Who Needs It |
|---|---|---|
| Single-Chamber Pacemaker | Paces right ventricle only | Simple bradycardia, AFib with AV block |
| Dual-Chamber Pacemaker | Paces both atrium and ventricle | Heart block, sick sinus syndrome |
| Biventricular Pacemaker (CRT) | Paces both ventricles simultaneously | Heart failure with dyssynchrony |
| ICD (Single/Dual Chamber) | Pacing + defibrillation | Cardiac arrest survivor, VT, cardiomyopathy |
| CRT-D | Biventricular pacing + defibrillation | Heart failure with arrhythmia risk |
| Phase | Duration | What to Expect |
|---|---|---|
| Immediate Post-Op | 4–6 hours | Bed rest, monitoring, chest X-ray |
| Hospital Stay | 1–2 days | Device testing, wound care instructions |
| First Week | 7 days | Limited arm movement, no heavy lifting |
| First Month | 4 weeks | Gradual return to normal activities |
| Long-Term | Lifelong | Regular device checks and monitoring |
If you have bradycardia, heart block, or are at risk for sudden cardiac death, device therapy could save your life. Consult our cardiac electrophysiology team at Primax Gastro Institute & Super Speciality Hospital. Call [9666460009] to schedule your evaluation.
What is Coronary Angiography? Angiography is a minimally invasive procedure where a thin catheter is inserted through your wrist or groin artery and advanced to your heart. Contrast dye is injected into coronary arteries while X-ray images (called angiograms) are recorded.
This creates a detailed roadmap of your coronary circulation, showing blockages, narrowing, or abnormalities.
Your Cardiologist Orders Angiography For:
| Procedure Type | Purpose | Access Site |
|---|---|---|
| Diagnostic Angiography | Visualize coronary arteries, identify blockages | Radial (wrist) or femoral (groin) |
| Ad-hoc Angioplasty | Diagnosis + treatment in same sitting if needed | Usually radial |
| Left Ventriculography | Assess left ventricle function, wall motion | With coronary angiography |
| Aortography | Evaluate aortic valve, aorta | With coronary angiography |
A. Pre-Procedure Preparation:
B. During the Procedure:
✅ Do’s:
❌ Don’ts (First 24–48 Hours):

The center is staffed by renowned dermatologists with 15+ years of specialized experience, certified cosmetologists for aesthetic treatments, and trichology experts specializing in advanced Hair Fall and Hair Transplant solutions.

Thank You for Submitting
You appointment query has been registered you will soon recieve confirmation call from Hospital if not received call@9666460009
