- Emergency Line:(+91) 9555943636
- Mon - Fri: 9:00 am - 5:00 pm (24x7 Emergency)
- 8 Marla, Model Town, Sonipat, Haryana 131001
Pain Management & Palliative Care

Welcome to the Pain Management & Palliative Care Department at Primax Gastro Institute & Superspeciality Hospital, Sonipat.
If you or your loved one are searching for lasting freedom from chronic pain, arthritis, or complex palliative needs, you’ve arrived at Haryana’s leading center for advanced solutions.
Our team combines world-class expertise, dedication to holistic care, and the latest interventions – empowering you to regain mobility, comfort, and quality of life.
From knee pain and joint distress to back pain and debilitating neuropathy, we deliver personalized plans for every patient’s journey.
With a strong emphasis on non-invasive techniques, medication optimization, and emotional support, our clinic ensures that patients receive respectful, empathetic, and comprehensive care at every stage of their journey.
✅ Unparalleled Pain & Palliative Expertise
✅ Next-Generation Facility & Technology
✅ Caring, Whole-Person Approach
✅ Caring, Whole-Person Approach
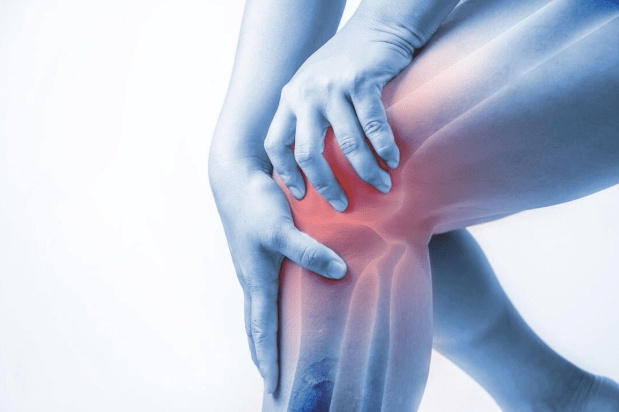
Knee pain and joint discomfort can drastically limit your independence. Whether caused by injury, arthritis, or overuse, our pain specialists in Sonipat offer advanced diagnostic and interventional therapies.
Symptom | Typical Cause | Recommended Action |
|---|---|---|
Morning stiffness | Arthritis | Book evaluation |
Swelling | Injury/arthritis | Consultation, imaging |
Locking/catching | Ligament or meniscus involvement | Orthopedic assessment |
Let us help you restore active movement with compassionate, cutting-edge care.
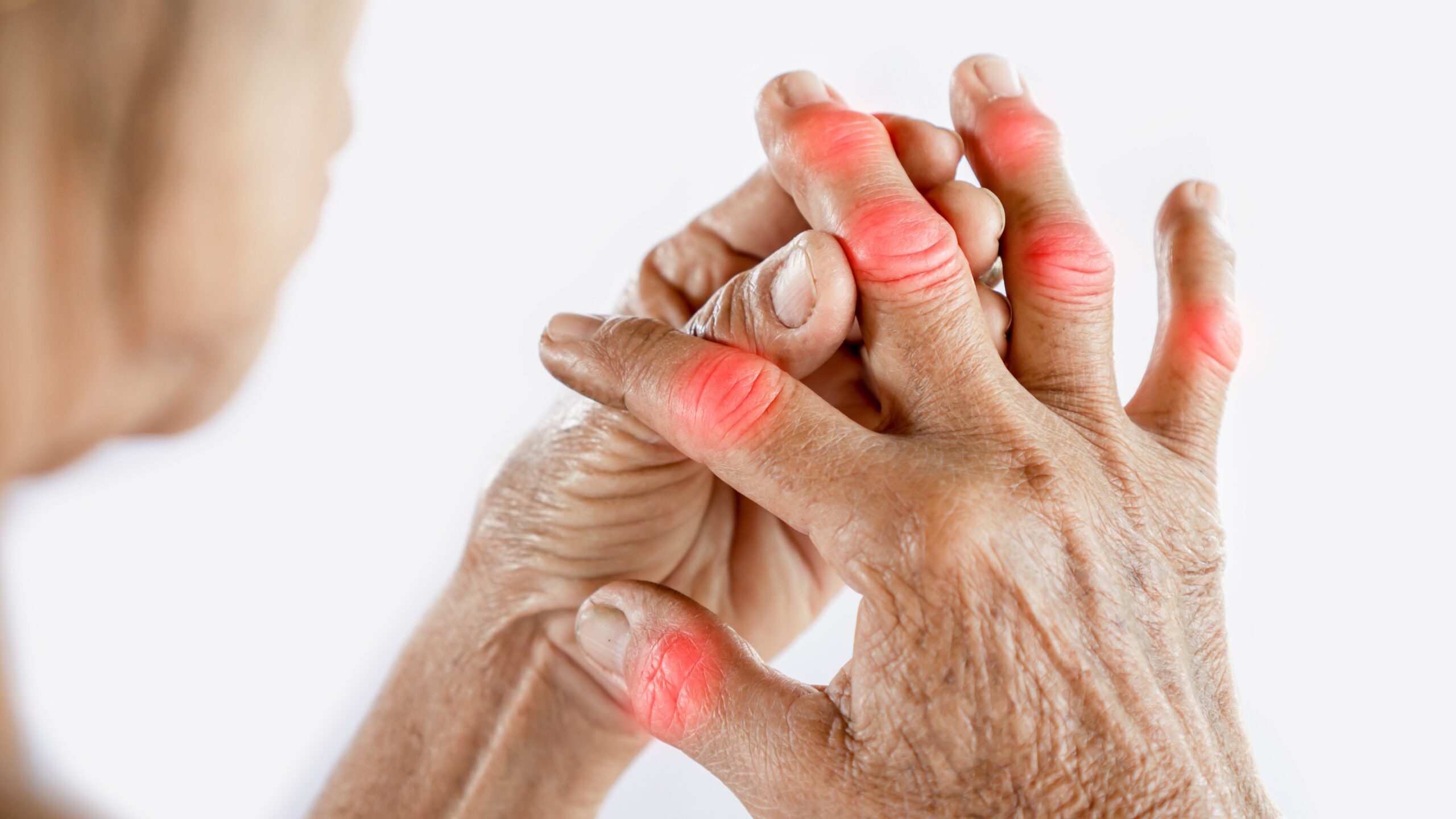
Arthritis is not just a disease of old age – it can strike anyone, affecting joints, comfort, and quality of life. Our pain management team employs a holistic, stepwise approach for different arthritis types.
Empower yourself with specialized arthritis care for pain-free living.
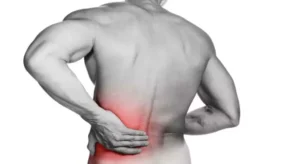
Chronic or sudden back pain often signals issues like sciatica or a slipped disc, impacting daily activity and sleep.
Don’t let back pain control your life – regain comfort and function with our expert team.
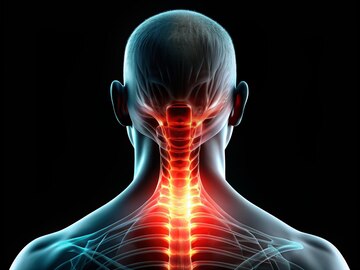
Neck discomfort, stiffness, or radiating pain may arise from cervical spondylosis, postural issues, or nerve compression.
Symptom Category | Description | Action Required |
|---|---|---|
Mild Stiffness | Occasional discomfort | Conservative care |
Moderate Pain | Daily pain, arm tingling | Comprehensive evaluation |
Severe | Shooting pain, weakness | Urgent care |
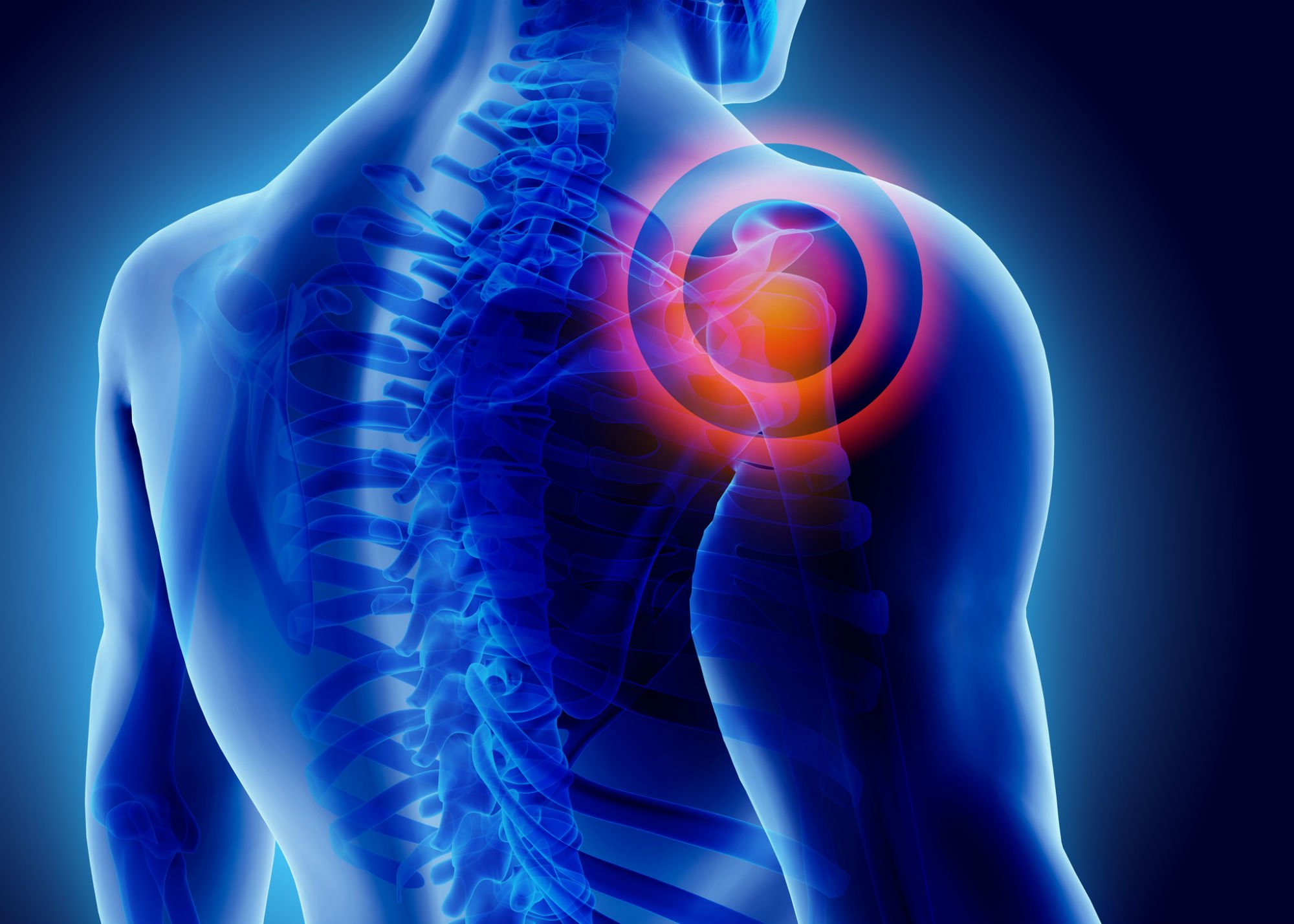
Shoulder pain and stiffness can make simple tasks difficult. Whether frozen shoulder or injury, our specialists restore function and eliminate pain.
Symptom Stage | Description | Action |
|---|---|---|
Freezing | Increasing pain, decreasing motion | Early intervention |
Frozen | Peak stiffness | Aggressive therapy |
Thawing | Gradual improvement | Continued rehab |
Athletes need specialized care for sports injuries and tendinitis. Our sports medicine approach ensures rapid relief and safe return to peak performance.
Injury Type | Characteristics | Treatment |
|---|---|---|
Acute Sprain | Sudden pain, swelling | RICE, mobilization |
Tendinitis | Activity-related pain | Anti-inflammatory |
Chronic | Persistent pain | Regenerative therapy |
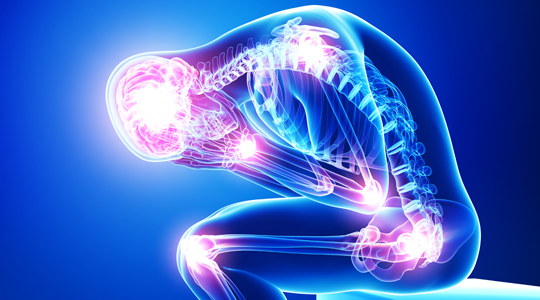
Fibromyalgia involves widespread musculoskeletal pain with abnormal pain processing in the brain. Triggers include genetic predisposition, infections, trauma, and central nervous system sensitization.
Symptom Category | Description | Action Required |
|---|---|---|
Early Signs | Mild widespread aching, occasional fatigue | Schedule consultation |
Moderate Impact | Daily pain, sleep issues, reduced activity | Comprehensive evaluation |
Severe | Debilitating pain, unable to work | Urgent care |
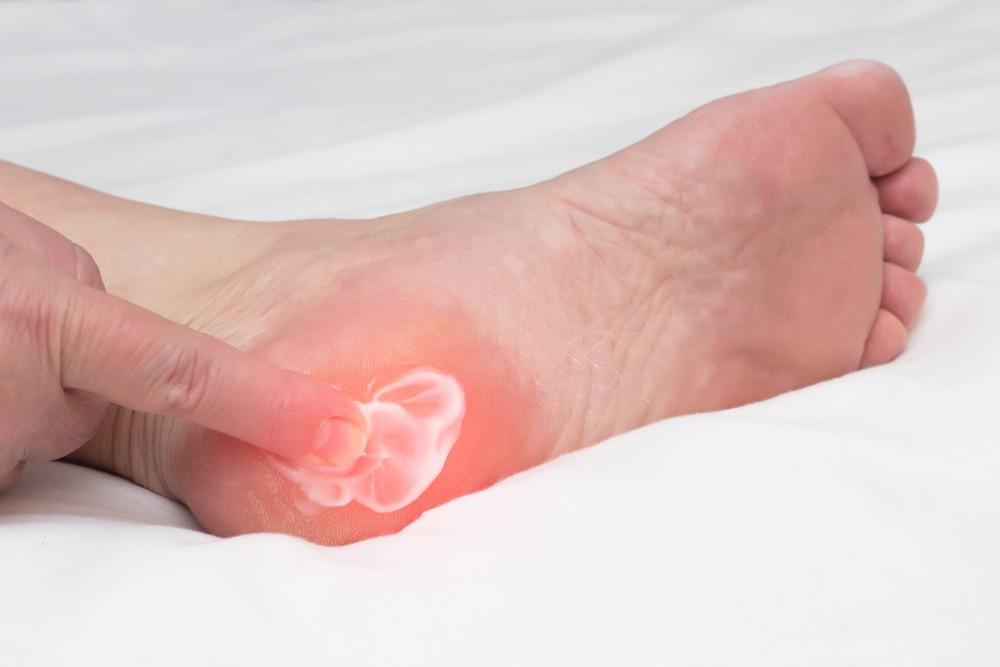
Every step shouldn’t hurt. Our specialists help you walk comfortably again through advanced diagnostics and targeted interventions.
Symptom Category | Description | Action Required |
|---|---|---|
Morning Discomfort | Sharp heel pain with first steps | Schedule evaluation |
Chronic Pain | Persistent pain weeks/months | Comprehensive assessment |
Acute Injury | Sudden severe pain | Emergency evaluation |
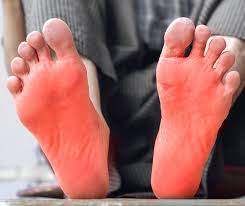
Nerve pain presents as burning, tingling, or shooting sensations that can be unbearable. Our specialized team targets the root cause for lasting relief.
Symptom Level | Description | Action |
|---|---|---|
Mild | Occasional tingling | Consultation |
Moderate | Daily burning pain | Immediate evaluation |
Severe | Debilitating pain, ulcers | Emergency care |
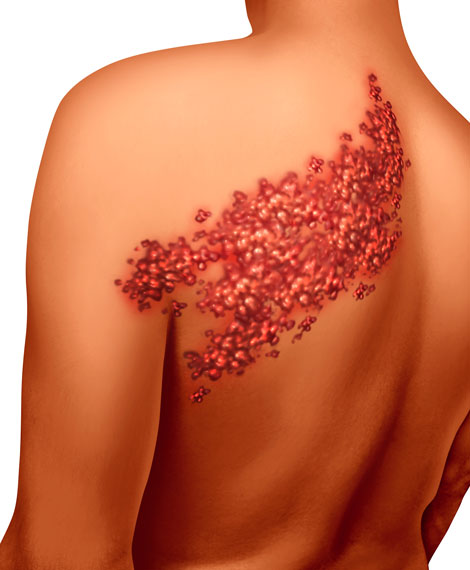
Persistent burning pain after shingles (herpes zoster) can severely impact quality of life. Our advanced therapies restore comfort and help you sleep peacefully again.
This condition occurs when nerve fibers are damaged during a shingles outbreak, causing chronic pain that persists after the rash heals. Risk increases with age and severity of initial shingles.
Pain Duration | Description | Treatment Approach |
|---|---|---|
Acute (0-3 months) | Recent shingles outbreak | Early intervention |
Subacute (3-6 months) | Persistent localized pain | Aggressive management |
Chronic (6+ months) | Established neuropathy | Multimodal therapy |
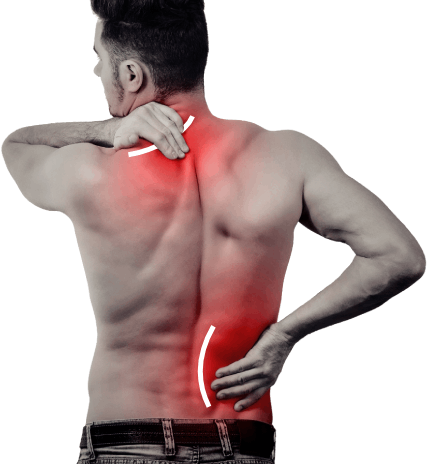
Muscle pain and myofascial trigger points create localized or referred pain that limits movement and reduces quality of life. Our targeted approach identifies and treats these painful areas effectively.
Pain Pattern | Location | Typical Treatment |
|---|---|---|
Localized | Single muscle group | Trigger point injection |
Regional | Multiple connected areas | Combined therapy |
Widespread | Multiple body regions | Comprehensive management |

Chronic headaches and migraines can be debilitating, affecting your productivity, relationships, and overall well-being. Our specialized headache clinic offers comprehensive diagnosis and cutting-edge treatments.
Headache Type | Characteristics | Treatment Focus |
|---|---|---|
Tension | Band-like pressure | Stress management, muscle relaxation |
Migraine | Throbbing, nausea | Preventive + acute medications |
Cluster | Severe one-sided, periodic | Oxygen, nerve blocks |
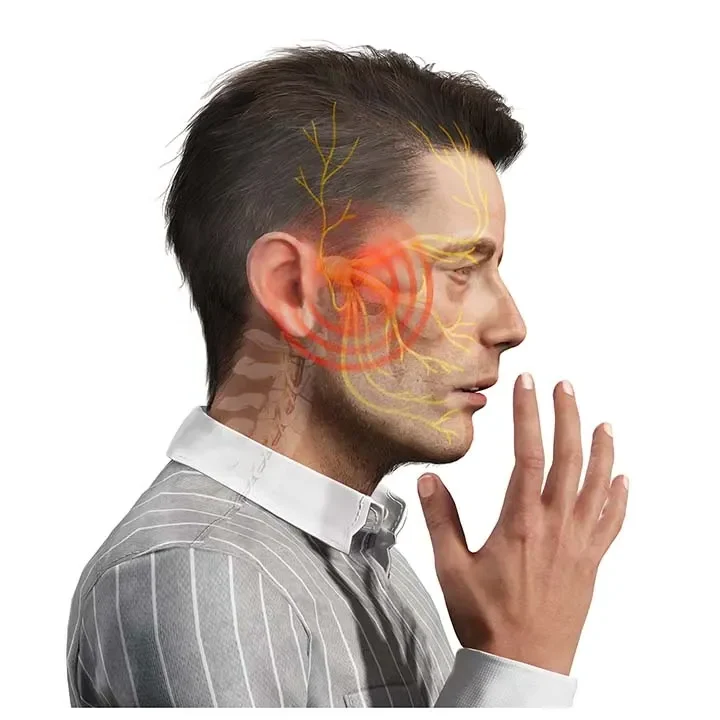
Trigeminal neuralgia causes sudden, severe facial pain often described as electric shocks. Our specialized interventions provide relief when medications alone aren’t enough.
This condition affects the trigeminal nerve (5th cranial nerve), causing intense facial pain triggered by everyday activities like eating, talking, or touching the face.
Pain Severity | Frequency | Treatment Stage |
|---|---|---|
Mild | Occasional episodes | Medication management |
Moderate | Daily episodes | Advanced medications |
Severe | Multiple daily attacks | Interventional procedures |
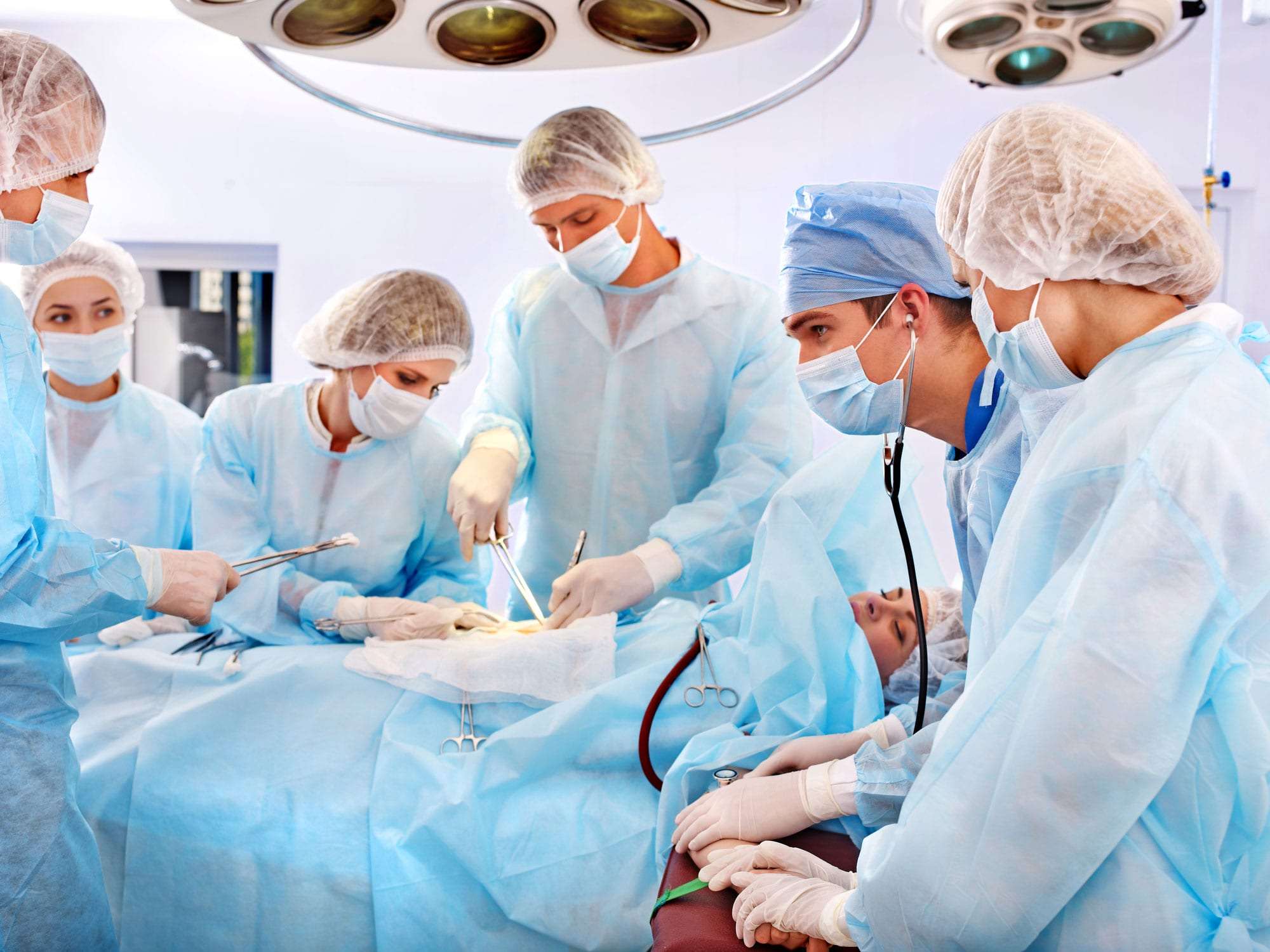
Persistent pain after surgery (lasting beyond the expected healing time) requires specialized attention. Our post-surgical pain clinic identifies causes and provides targeted solutions for complete recovery.
Time Post-Surgery | Pain Status | Action |
|---|---|---|
0-3 months | Acute post-op pain | Standard pain management |
3-6 months | Prolonged pain | Specialized evaluation |
6+ months | Chronic post-surgical pain | Comprehensive intervention |
Procedures
Epidural injections
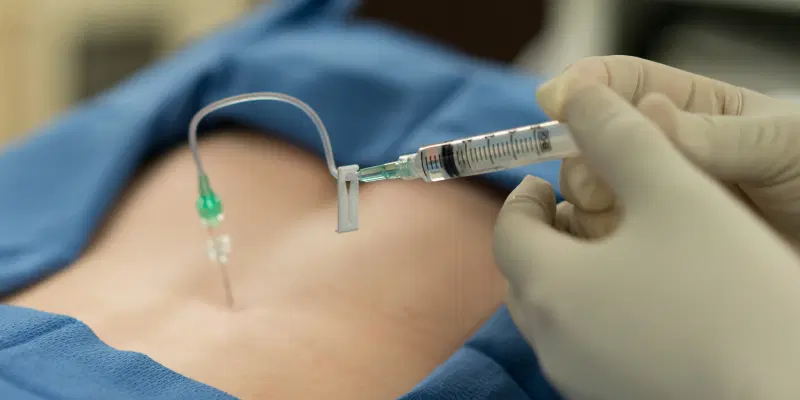
Epidural injections (cervical, thoracic, lumbar, caudal): Epidural injections are used to deliver medication directly into the epidural space around the spinal cord to relieve pain from conditions like herniated discs, sciatica, or spinal stenosis. They help reduce inflammation and provide pain relief.
Purpose: Direct medication delivery to spinal nerves
Treats:
Benefits:
✅ Reduces nerve inflammation
✅ Minimally invasive
✅ Avoids surgery in many cases
✅ Image-guided for precision
✅ Lasting relief for weeks to months
Facet joint injections and medial branch blocks
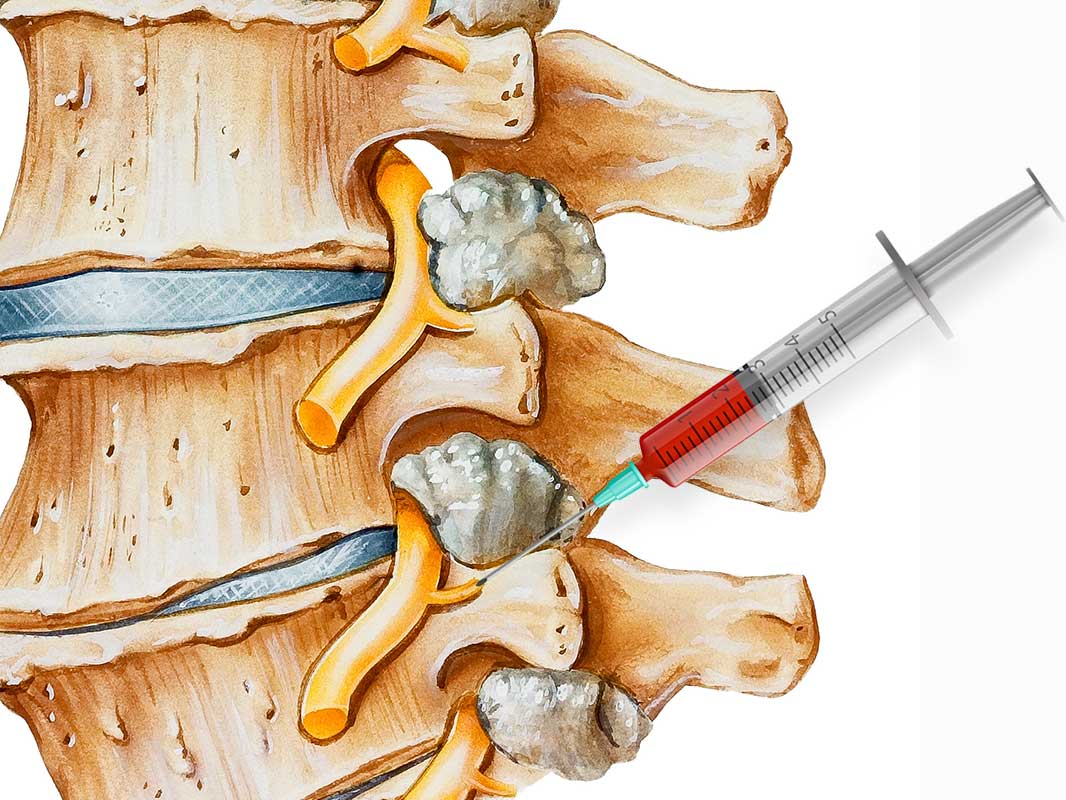
Facet joint injections and medial branch blocks: Facet joint injections involve injecting medication into the small joints of the spine to relieve pain caused by arthritis or injury. Medial branch blocks target the nerves that supply these joints, providing temporary pain relief to diagnose and treat back pain.
Purpose: Target inflamed spine joints
Ideal For:
What We Do:
✅ Inject anesthetic + steroid medication
✅ Diagnose exact pain source
✅ Provide therapeutic relief
✅ Relief lasts weeks to months
✅ Outpatient procedure
Radiofrequency ablation (RFA)
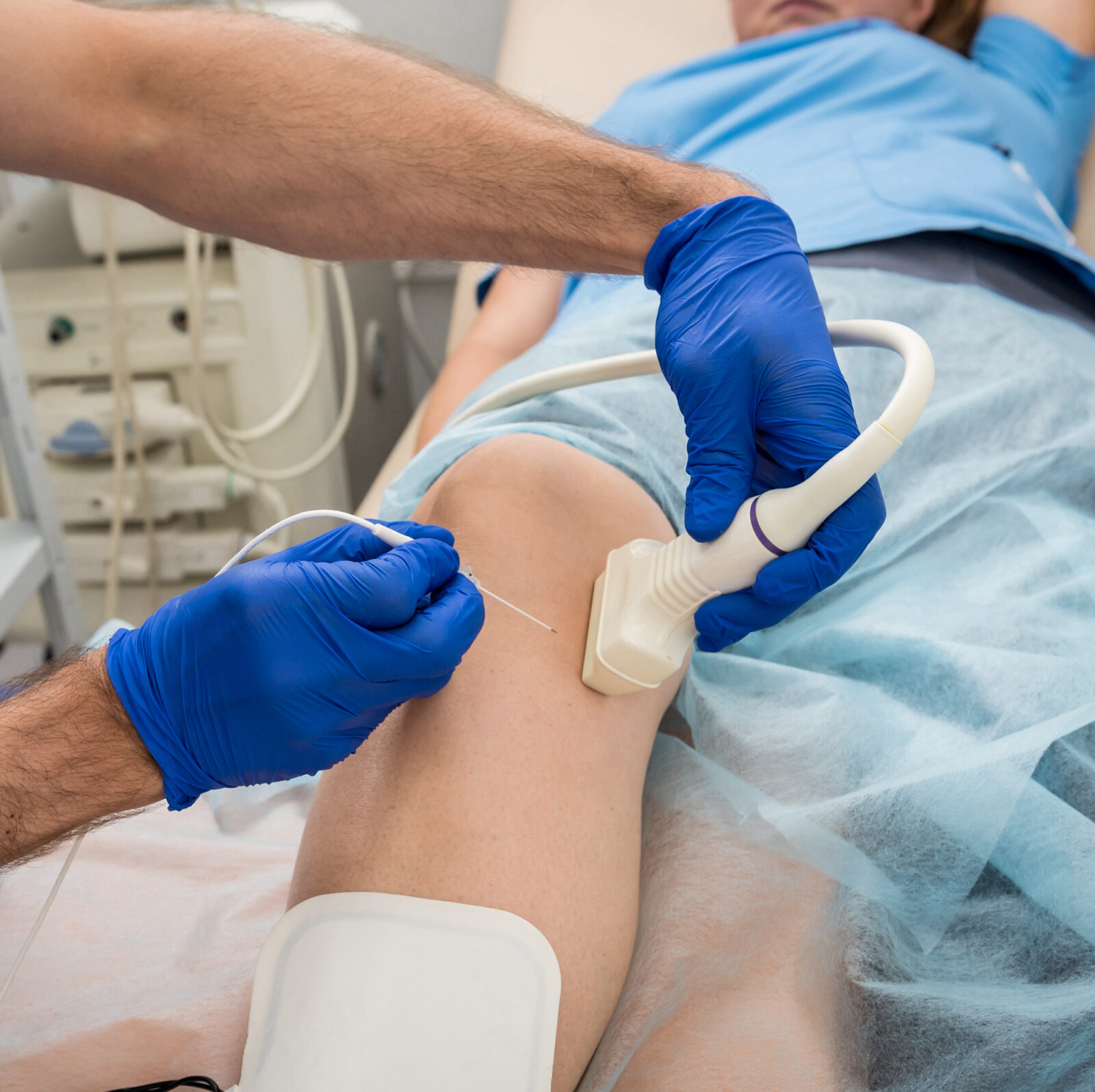
Radiofrequency ablation (RFA) for chronic pain: Radiofrequency ablation is a minimally invasive procedure that uses heat to target and disable specific nerves responsible for pain. It’s commonly used to treat chronic back, neck, or joint pain, especially when other treatments have failed.
How It Works: Heat disrupts pain-transmitting nerves
Best For:
Key Advantages:
✅ Long-lasting relief (6-12+ months)
✅ Minimally invasive
✅ Quick recovery
✅ Significantly improves quality of life
✅ Repeatable if needed
Sacroiliac joint injections
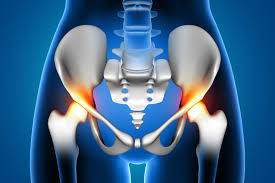
Sacroiliac joint injections: A sacroiliac joint injection involves injecting medication into the sacroiliac joint to reduce inflammation and provide pain relief. It is commonly used to treat lower back and pelvic pain caused by sacroiliac joint dysfunction or arthritis.
Target Area: SI joint (spine-to-pelvis connection)
Common Symptoms:
Procedure Benefits:
✅ Confirms pain source
✅ Reduces inflammation
✅ Immediate diagnostic value
✅ Therapeutic relief
✅ Precision-guided injection
Sympathetic Nerve Blocks
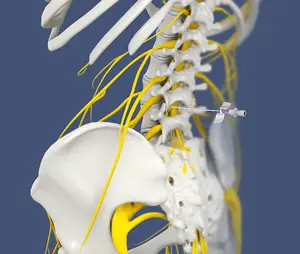
Sympathetic nerve blocks (stellate ganglion, lumbar sympathetic, celiac plexus, etc.): Sympathetic ganglion blocks involve injecting anesthetic near specific nerve clusters (sympathetic ganglia) to interrupt pain signals. These are used to treat chronic pain conditions, such as complex regional pain syndrome (CRPS) or vascular pain.
Specialized For: Complex nerve pain conditions
Primary Uses:
What It Relieves:
✅ Burning pain
✅ Abnormal sweating
✅ Temperature changes
✅ Skin color changes
✅ Chronic nerve hypersensitivity
Peripheral nerve blocks
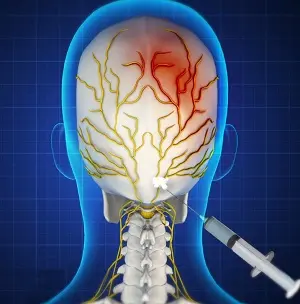
Peripheral nerve blocks: Nerve blocks involve injecting medication near specific nerves to block pain signals from reaching the brain. They are used to manage chronic pain, provide temporary relief for acute pain, and assist in diagnosing the source of pain.
Purpose: Block specific nerve pain signals
Conditions Treated:
Advantages:
✅ Immediate pain relief
✅ Diagnostic + therapeutic
✅ Targeted approach
✅ Minimal side effects
✅ Combines well with physical therapy
Trigger Point Injections
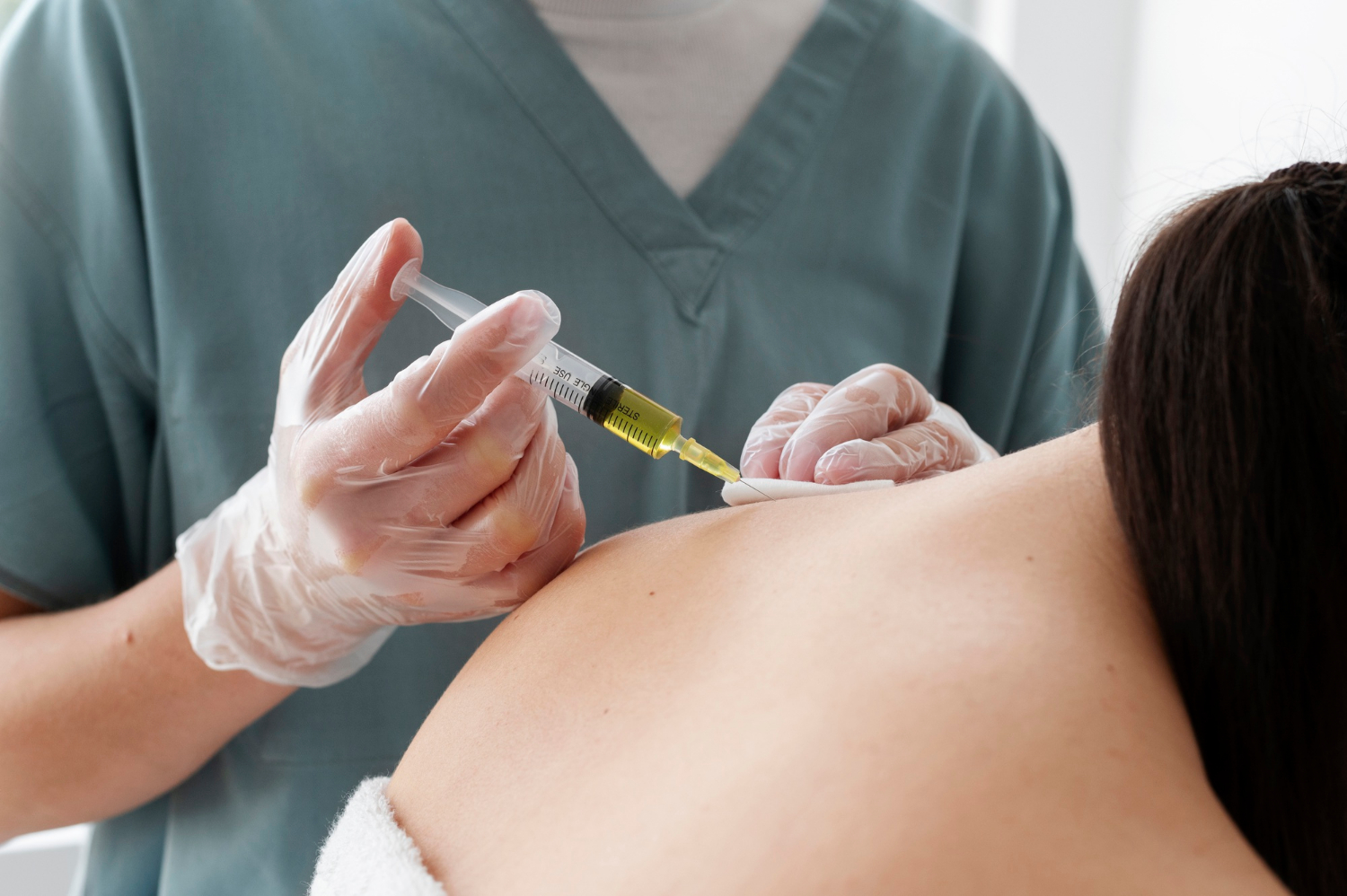
Trigger point injections: Trigger point injections involve injecting medication directly into muscle knots (trigger points) to relieve pain, reduce muscle tightness, and improve mobility. They are commonly used to treat conditions like myofascial pain syndrome.
Target: Painful muscle knots and tight bands
Effective For:
Treatment Approach:
✅ Direct anesthetic injection
✅ Releases muscle tension
✅ Immediate relief
✅ Combined with stretching
✅ Quick outpatient procedure
Platelet-Rich Plasma (PRP) and Regenerative Therapies
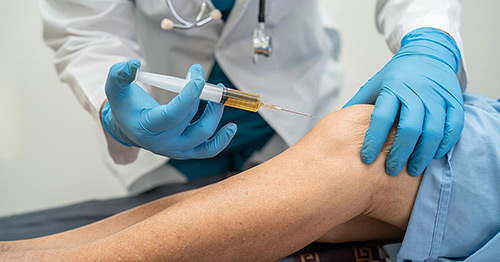
Platelet-rich plasma (PRP) and regenerative therapies: PRP treatment involves injecting a concentrated solution of the patient’s own platelets into an area of injury or pain to promote healing. It is commonly used for tendon, ligament, and joint issues, including osteoarthritis and sports injuries.
Benefits: Non-surgical, promotes natural healing, long-term relief
Uses Your Own Blood’s Healing Power:
Treats:
✅ Tendinitis (Achilles, rotator cuff, tennis elbow)
✅ Ligament injuries
✅ Arthritis
✅ Sports injuries
✅ Chronic joint pain
Prolotherapy
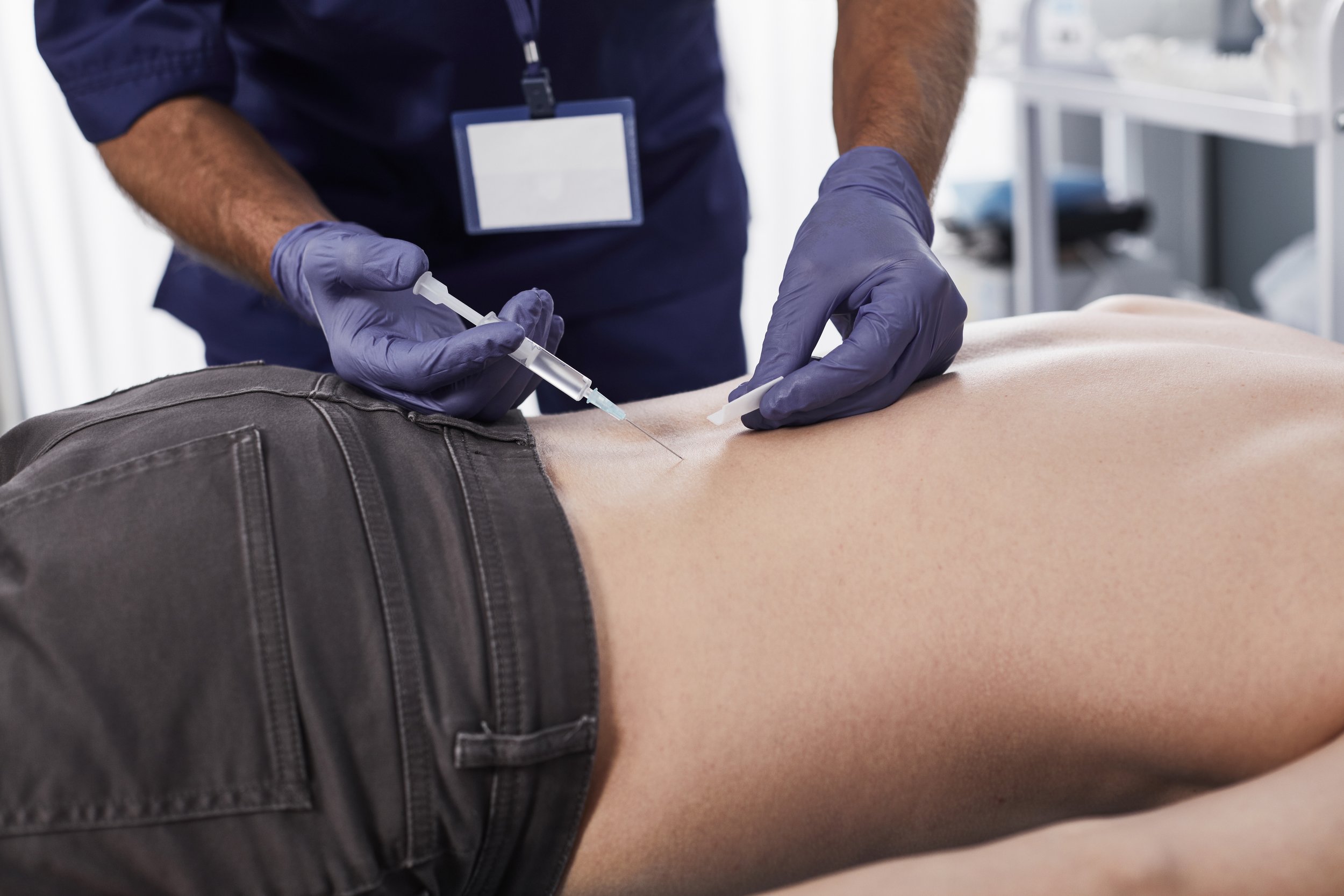
Prolotherapy: Prolotherapy is an injectable treatment that involves using a sugar solution to stimulate the body’s healing process. It promotes tissue repair and is often used to treat ligament or tendon injuries, as well as joint pain and instability.
How It Works:
Best For:
✅ Chronic joint instability
✅ Ligament laxity
✅ Tendon weakness
✅ Sports injuries
✅ Arthritis pain
Outcome: Stronger tissues, stable joints, reduced pain
Botox Injections for Migraine, Myofascial Pain
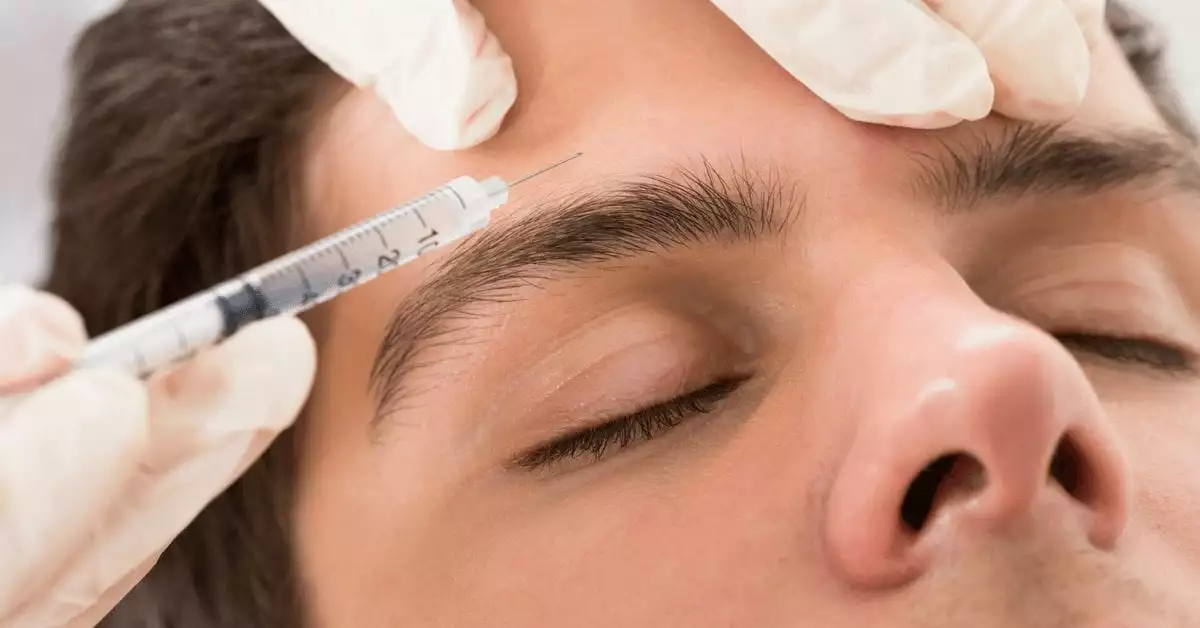
Botox injections for migraine, myofascial pain: Botox injections can be used to treat chronic pain conditions, such as migraines, muscle spasms, and temporomandibular joint (TMJ) disorders. The botulinum toxin blocks nerve signals that trigger pain, providing relief for some patients.
FDA-Approved Chronic Migraine Prevention
Who Benefits:
Treatment Details:
✅ Injected at specific head/neck sites
✅ Every 12 weeks
✅ Blocks pain signals
✅ Reduces frequency & severity
✅ Proven long-term safety
Results: Fewer migraine days, improved quality of life
Intrathecal Drug Delivery Systems
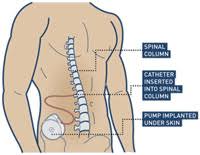
Intrathecal drug delivery systems: The intrathecal drug delivery system involves implanting a pump to deliver pain-relieving medication directly into the spinal fluid. This targeted treatment is used for chronic pain that doesn’t respond to other therapies, such as severe back pain or cancer pain.
For Severe, Intractable Pain:
How It Works:
✅ Implanted pump device
✅ Direct spinal fluid medication delivery
✅ Minimal doses needed
✅ Maximum pain control
✅ Reduced systemic side effects
Discography and Intradiscal Procedures

Discography and intradiscal procedures: Discography is a diagnostic procedure where contrast dye is injected into the spinal discs to assess disc integrity and identify the source of back pain. It helps determine if a disc is causing pain, especially when other tests are inconclusive.
Discography Purpose:
Intradiscal Procedures:
✅ Minimally invasive disc treatment
✅ Pinpoints exact pain source
✅ Alternative to major surgery
✅ Image-guided precision
✅ Faster recovery
Customized Physical Therapy and Rehabilitation-based Pain Treatment

Physical therapy and rehabilitation-based pain treatment: Physical therapy and rehabilitation focus on restoring movement, strength, and function after injury or surgery. It involves exercises, manual therapy, and education to manage pain, improve mobility, and prevent future injuries.
Our Approach Includes:
Goals:
✅ Restore full function
✅ Improve mobility
✅ Prevent future injuries
✅ Build strength
✅ Long-term pain management
✅ Return to normal activities
Lifestyle Modification and Integrative Pain Care

Lifestyle modification and integrative pain care: Lifestyle modification involves making changes to daily habits, such as improving diet, increasing physical activity, managing stress, and quitting smoking. These adjustments can help prevent or manage chronic conditions like pain, arthritis, and cardiovascular disease.
Areas We Address:
Personalized Strategies For:
✅ Weight management
✅ Smoking cessation
✅ Pain trigger identification
✅ Activity modification
✅ Sustainable pain relief
✅ Overall health improvement

Book online via the Contact Us page, use the ‘Book Appointment’ or ‘ChatNow’ buttons, or call 9666460009. Our coordinators will assist you immediately.
Please bring your prior medical records, scans, current medications, and a list of symptoms and their duration.
We treat all acute and chronic pain, including neck/back/knee pain, arthritis, neuropathy, migraine, post-operative pain, and palliative care needs.
Yes! We have a 24/7 emergency support line at 9666460009 for urgent interventions and admissions.
Our experts perform epidural injections, nerve blocks, radiofrequency ablation, advanced physiotherapy, regenerative therapies (PRP & Prolotherapy), and more as clinically appropriate.

Thank You for Submitting
You appointment query has been registered you will soon recieve confirmation call from Hospital if not received call@9666460009
